Pediatric nurses provide health and medical care for children from birth through their late teens. These nurses have special training to provide expert care to the child while working with the family to address their concerns, problems, and to help them understand treatment options. They also work closely with pediatricians and other medical specialists involved in treating the patient.

Becoming a pediatric nurse takes a combination of loving kids and being strong in the face of their suffering.
There are no patients that are more difficult to care for than kids. Whether they are infants who can’t tell you where it hurts other than by screaming, or teenagers who believe they are immortal, kids bring challenges to the practice of medicine on top of the constant difficulties of treatment. On top of that, pediatric nurses are never really dealing only with kids. Parents are a constant presence, and often a distracting one.
That means pediatric nurses, and especially advanced practice pediatric nurses, have to develop a unique set of capabilities in communication and treatment techniques. Working with patients who may not even be able to talk yet requires unique diagnostic insight. Even older kids might not have the vocabulary or experience to tell you exactly what is wrong. You have to develop mind-reading as well as treatment skills!
Pediatric Nurse Practitioner Jobs: PNP Job Description
Can a Family Nurse Practitioner Work in Pediatrics?
What Does a Pediatric NP Do in a Typical Day?
What Are Pediatric NP Responsibilities and Duties?
The Differences in Pediatric Primary Care Vs Acute Care Nurse Practitioner Jobs
Facts and FAQs About Pediatric Nurse Practitioners
But because individuals with those abilities are so rare, they are also highly prized. You may be one of the few with the talents to put advanced nursing skills to good use among a population that deserves the best kind of care. You owe it to them and yourself to get the best training you can on that path.
The Difference Between Pediatric Nurses and Pediatric Nurse Practitioners
Not all nurses working in the pediatric ward are just pediatric nurses. Although all of them will answer the call when someone is looking for a nurse, there’s a big difference between RN (Registered Nurse) ped staff and APRN (Advanced Practice Registered Nurse) staff in the unit.
RNs typically have four-year bachelor’s degrees and have passed the necessary NCLEX-RN national licensure exam. Peds nurses also commonly obtain specialty certification in the form of the Certified Pediatric Nurse (CPN) credential from the Pediatric Nurse Certification Board (PNCB).
In contrast, APRNs must hold a master’s degree or higher. That means at least six, and often eight or more years of advanced training. That training is also specific to pediatric practice, unlike the more general training RNs receive. Most APRNs also have experience as RNs prior to going through that advanced training, so they have practical knowledge and skills in nursing already.
This means that pediatric NPs are trained and prepared to deliver some kinds of care that in the past only doctor’s have been able to provide. Pediatric RNs provide valuable patient care and support to both, but do not deliver the advanced procedures that NPs and doctors perform.
Pediatric Nurse Practitioner Jobs: PNP Job Description
The unique blend of advanced medical knowledge and expert nursing skills that a pediatric nurse practitioner brings to the table means taking on a lot of tasks in peds wards. You have the holistic perspective of the nursing world combined with the diagnostic and treatment skillset approaching that of MDs. That qualifies you to handle a lot of different job duties. Hospitals aren’t slow to take advantage of that kind of flexibility.
PNPs in different specialty areas can take on very different types of tasks. In general, though, pediatric nurse practitioners share a certain practical set of job duties:
- Monitoring and updating basic child wellness – Although pediatric NPs can perform many advanced procedures, the basic grounding in the nursing tradition means they always have an eye on the fundamentals. PNPs share a responsibility for understanding and addressing all the healthcare needs of a patient, even those originating outside their own specialty area.
- Physical exams and diagnostics – One area where PNPs excel is in handling physical examinations and making diagnoses of younger patients. The nursing approach to care is particularly well-suited to working with children, who may not understand, and can be frightened by, the dispassionate medical approach. PNPs know how to break the ice with empathy and communication to get the data they need without further traumatizing already sick kids.
- Acting as care coordinators and communicators with families and medical staff –Pediatric APRNs also have an edge when it comes to communication. Their high-level medical knowledge comes together with a ground-level view of what is going on with patients and families in the ward. That puts them in a unique perspective for explaining arcane procedures to families, communicating patient and family concerns to doctors, and even approaching administration with needs and concerns out on the floor. A good PNP is approachable and engaged with both patients and medical professionals.
- Referring patients to other appropriate resources in the hospital and in the community – PNPs also know when they are running into areas that are outside their expertise. They serve as a central resource for patients and providers who need to bring in other experts to handle non-medical, or even more highly specialized treatment resources. That can range from contacting a social worker to help arrange for subsidized in-home care for a patient after discharge to referring a kid with psychological issues to a psychiatrist even after their physical problems have been treated.
- Handling patient comfort and mental well-being – No one gets into pediatric nursing without a big helping of empathy and understanding. You have to love kids, and when you love kids, you will go the extra mile to ease their pain and anxiety. That can mean everything from handing out hugs to just sitting and chatting about an upcoming procedure to arranging for access to a video game console in a patient’s room. Knowing what is needed and going out of your way to get it is all part of the job for a pediatric nurse practitioner.
- Providing direct care for illness and injury – Of course, the largest part of the job is in direct care. You will attend school for six or more years to develop the patient care skills required of a PNP, and you will spend most of your career putting them into practice. Performing general and specialized procedures is the most important thing you can offer to reduce suffering and send your patients on to a happier and healthier life.
- Offering counseling and advice – PNPs don’t just offer hugs and well-wishes. You are sitting on a wealth of medical and healthcare knowledge that you can use to help both patients and their families through conversation and counseling. In many cases, this can be direct healthcare knowledge, basic things like how to change a dressing. But it can also extend to other things that people don’t normally understand, ranging from medical billing to coping with the mental hardship of a loved one’s chronic illness.
The day-to-day details of this work can involve combinations of clinical and administrative work. You’ll be expected to have solid charting skills and an excellent bedside manner.
The role of a pediatric NP depends in some part on their place of employment and the state where they are working.
- In doctor’s offices or private practice – Primary care PNPs offer long-term, comprehensive, and continuous care to patients. They monitor overall health status, track developmental progress, and keep up immunization and other basic wellness treatments.
- In hospital pediatric wards – PNPs in hospital settings may offer primary care similar to doctor’s offices, but often work in acute care. They diagnose and treat critically ill, unstable, and vulnerable children in emergency rooms or PICU (Pediatric Intensive Care Unit) or NICU (Neonatal Intensive Care Unit) wards. They usually work as an important part of an interdisciplinary care team.
- In community health centers – PNPs in community health care get a mix of roles, ranging from public health surveillance to primary care treatments to handling the occasional acute care case that may walk in the door. They engage a lot with patient families and keep a finger on the pulse of the community as part of holistic care efforts.
- In surgery centers – PNPs in surgical settings usually serve as the primary assistant to surgeons who are operating on pediatric cases. They are responsible for monitoring the procedure, performing basic procedures like wound site closure and dressing, and handling technical elements of the surgery.
Because fewer than half of states offer pediatric nurse practitioners the authority to practice independently, many of those positions will require collaborative practice agreements and supervision at some level from a medical doctor. In states with independent practice laws, though, peds NPs can deliver care without consultation, or even operate their own private practice.

Can a Family Nurse Practitioner Work in Pediatrics?
Family nurse practitioners treat patients of all ages, which creates some definite overlap with the job role of a pediatric nurse practitioner. In fact, in some pediatric practices you will find FNPs and PNPs working side by side.
Family nurse practitioners are a more generalized role, while pediatric nurse practitioners are considered more highly specialized.
As an FNP, you can pick the patient population that you want to work with, from childhood to adulthood. So in some sense, FNPs can and do work in pediatrics all the time.
They are not specialists in the same way that PNPs are, however. The extra training in acute or primary care that is a part of a pediatric NP’s education isn’t found in FNP programs. That means FNPs aren’t suitable for some kinds of pediatric care treatment. Family nurse practitioners are not eligible for certification as pediatric NPs without additional specialized education in the subject.
The path from FNP to PNP is common enough, however, that the PNCB offers a complete page on FNP-to-PNP certification guidance for a step-by-step process.
What Does a Pediatric NP Do in a Typical Day?
A day in the life of any pediatric nurse can be vastly different depending on their role. But there are some common elements that almost every PNP goes through in the typical day.
Maybe it’s not surprising that perhaps only teachers spend more of their time with kids than you will as a PNP.
Unfortunately, it’s not all play. Those kids are sick, and a lot of the day for a PNP will be spent figuring out what is wrong and how to fix it. The first part can be the hardest. Your patients aren’t at an age where communicating their pain and symptoms are easy yet.
How Pediatric Nurse Practitioners Work With Children
One of the toughest skills you’ll master for daily use as a PNP is how to communicate with and treat kids effectively and efficiently. It’s something you have to practice, but the techniques are pretty basic:
- Put yourself physically on the same level as kids… towering over them is intimidating!
- Smile, smile, smile! Kids are conditioned early to respond to simple signs of friendliness.
- Enlist the patient in the treatment. Whether it’s helping to hold some gauze or watching a number on your BP cuff, it’s new to your patient and offers a distraction.
- Keep it real when you talk; kids can spot a fake a mile off and you’ll never get your credibility back if you tell them it’s not going to hurt and then it does.
- Ask them questions! You can show you care in ways they can understand, and curiosity is a great one.
Managing fear is far more important with kids than adult patients, so PNPs go the extra mile to be friendly, reassuring, and keep their patients calm even in the worst circumstances.
You also get the tough job of talking with parents about their child’s illness. Nurse practitioners are expert communicators, but you are talking with someone about the most important thing in their life and usually when there is something wrong. It takes tact and empathy to get through to parents in that position.
One big thing about working with kids all day is the excitement and sense of fun you get to bring to the job. Even though you’re dealing with some very serious situations and often some very sick children, part of your job is keeping their mind off of those problems. You get to wear bright scrubs, bring stuffed animals and cartoon Bandaids on your rounds, and prescribe lollipops along with codeine.
But you still spend a lot of the day doing nursing things… updating charts, monitoring equipment, making rounds, distributing medications, performing procedures. You communicate with colleagues, confer with specialists. Sometimes you will be on the phone, coordinating discharge and care plans, and other times you’ll be in meetings.

What Are Pediatric NP Responsibilities and Duties?
Of course, your day on the job can depend quite a bit on what type of job you are doing. Responsibilities and duties for NPs vary a lot based on specialization. That can make your day radically different from the typical NP.
Some of the more common job duties for pediatric NPs can include:
- Neonatal care duties – Working with the tiniest, most vulnerable infants takes a lot of attention to detail. The role routinely requires:
- Monitoring vitals for NICU patients
- Educating and training families of premature infants in transitional and home care
- Keeping staff and families up on patient developmental progress
- Monitoring and adjusting specialized equipment like capnographs, bilirubinometers, and ventilators
- Developmental care duties – PNPs in development care offer support for kids with mental and physical disabilities. Their tasks can include:
- Assisting in feeding and bodily functions
- Educating, training, and supporting parents in care for their child
- Assisting with the development of language and communication skills, in coordination with specialists
- Prescribing, monitoring, and maintaining assistive equipment
- Palliative care duties – Working with terminally-ill children takes vast reservoirs of empathy and willpower. But fulfilling these duties makes those last days better for both kids and their families:
- Communicating with families about patient status and progression
- Coordinating end-of-life care and processes with other specialists
- Monitoring physical and mental states
- Managing pain by appropriately delivering medications
- Primary care duties – Handling the day-to-day needs of ensuring a healthy generation means watching your patients grow from toddlers to teenagers. Primary care involves the full range of challenges that come at every age, from offering inoculations to counseling kids about STDs
- Examine and note vital statistics and any unusual symptoms or developmental issues
- Keep accurate charting and monitor growth against standards for each age
- Handle treatment of common childhood illnesses and injuries
- Make referrals to outside specialists and coordinate care for patients
The Differences in Pediatric Primary Care Vs Acute Care Nurse Practitioner Jobs
There’s a big divide in the pediatrics nursing world between primary care and acute care roles.
- Primary Care – Primary care nursing focuses on long-term health and well-being through services such as health promotion, screening, education, and preventative procedures. They tend to keep regular schedules and appointments in hospitals, clinics, and doctor’s offices.
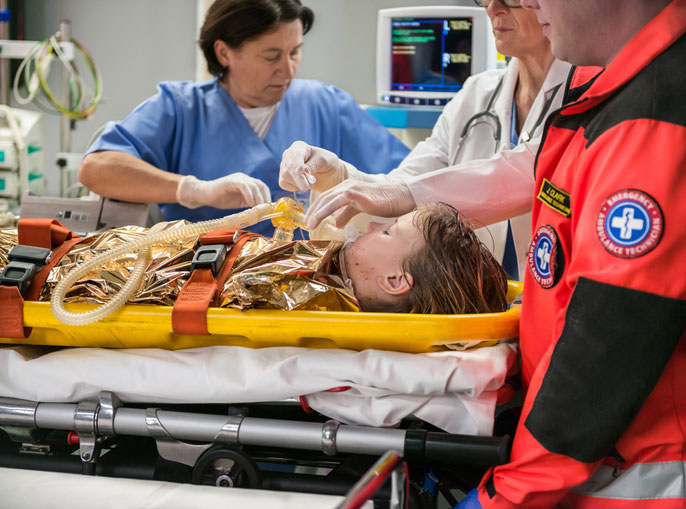
- Acute Care – Acute care nurses work with critical, immediate healthcare issues, handling some of the sickest patients in environments like intensive care units and emergency departments. They are most likely to work for hospitals or in skilled nursing facilities.
This divide is so fundamental that the certifications for the two jobs are different, and even the degrees offered in each have very specialized classes.
Although official data doesn’t differentiate between the two types of jobs, some salary surveys find that acute care specialists tend to make more money at any given level of experience. Considering the nature of acute care work and the hours involved, higher pay levels seem likely.
What is Work as a Pediatric Oncology Nurse Practitioner Like?
If you want to know what the hardest job in pediatric nursing is, you don’t have to ask around much to find the answer. Just about everyone agrees that pediatric oncology represents the toughest work in the nursing profession. Maybe it’s the hardest thing in healthcare.
Cancer is an awful disease, the body tearing itself to pieces at the cellular level. It’s hard to watch anyone suffering through it, but when it’s kids, the built-in empathy and protectiveness we feel kicks in to overdrive.
Even worse for pediatric oncology NPs is the fact that some of the treatments for cancer can be nearly as awful as the disease. To save those kids in your ward, you’re going to have to help poison them: chemical cocktails that devour cancer cells and at the same time hair follicle cells. Radiation that zaps healthy cells and tumors without discretion. It’s heartbreaking, but it’s also where the hope comes from. And having that hope in your hands can also be a powerful feeling, one that makes the bad days worthwhile.
Facts and FAQs About Pediatric Nurse Practitioners
You’re going to have a lot of questions about becoming a pediatric nurse practitioner. Here, you’ll find some answers to many of those most common questions.
What is the age range of patients treated by pediatric nurse practitioners?
Pediatric nurse practitioners treat patients from infancy through young adulthood. The specific scope of practice authorized for PNPs varies from state to state. In some cases, the cut off may be at ages 18 or 21, but in other states, no specific number is determined. In general, it’s best for medical providers to agree on who can offer the best care in any specific case.
Do I need a certification to practice as a pediatric nurse practitioner?
Yes, in nearly every state you are required to hold a current certification from a recognized national credentialing body in order to become licensed as a pediatric nurse practitioner. For pediatric advanced nursing practice, that means a certification from the Pediatric Nursing Certification Board.
What is the Pediatric Nursing Certification Board and why is it important for pediatric nurses?
PNCB is the only remaining profession certification body covering the specific field of advanced practice pediatric nursing. Established in 1975, they have established a level of competence and expertise in evaluating skill levels of prospective PNPs that makes them widely recognized as the standard-bearer for professionals in this field.
What certifications are available for pediatric nurse practitioners?
PNCB offers two different certifications for pediatric nurse practitioners:
- Acute Care Certified Pediatric Nurse Practitioner (CPNP-AC)
- Primary Care Certified Pediatrics Nurse Practitioner (CPNP-PC)
Just like it appears, these advanced practice certifications split between the kinds of knowledge and practices required in primary care versus acute care settings. Both require an MSN, DNP, or post-graduate certificate, 500 hours of direct clinical patient care hours, a current RN license, and passing a 175 multiple-choice question test. Your educational background also has to align with the certification you are pursuing, either acute or primary.
You might already have, or might choose to get, a CPN (Certified Pediatric Nurse) from the board also. It’s available to any nurse, not just APRNs, but covers a great deal of practical pediatric nursing knowledge.
Where do pediatric nurse practitioners work?
According to the Bureau of Labor Statistics, most nurse practitioners work in the offices of physicians or general medical and surgical hospitals.
That definitely holds true for PNPs. The advanced skills required for the job are a good match to the demands of a pediatrics ward or for general pediatric practice. But you can also find jobs for PNPs in:
- Surgery centers
- Pediatrician’s offices
- Community health centers
- Long-term care centers
- Ambulatory care centers
How can I become a pediatric nurse practitioner?
Like all advanced practice registered nurses, PNPs have to go through advanced training on top of the regular nursing education needed by registered nurses. A master of science in nursing is a path to advanced practice licensure, with an emphasis in pediatrics, but you can also go for a doctorate in nursing.
Additionally, you have to study topics such as:
- Pediatric development and behavior
- Pediatric disease management
- Advanced health assessment and diagnostics
- Advanced pathophysiology
- Pharmacology
On top of that, you’ll have courses that are unique to your sub-specialization in acute or primary pediatric care. And you’ll also take part in practicum placements to give you hands-on experience working with pediatric patients.
Can an online program qualify you as a pediatric nurse practitioner?
Yes, there are many excellent MSN and DNP programs that are conducted primarily online today with pediatric nurse specializations available. Of course, in healthcare, no program is truly entirely online. Your hands-on field experience must still be conducted in a local hospital or clinic. But all your coursework can be completed through asynchronous, online classes that allow you the maximum flexibility in your schedule and location.
Can APRNs from a different specialization become pediatric nurse practitioners?
Yes, but you will have to complete a post-master’s certificate program to get the same specialized coursework as ped NPs who come up through a dedicated MSN or DNP program. Just like those degree programs, you will have to choose between acute and primary emphasis in pediatric advanced practice nursing. And just as with full degree programs, you can find post-master’s certificate options available online.
What are the admissions requirements for pediatric nurse practitioner MSN and DNP programs?
Admissions requirements are rigorous for PNP education tracks. In most cases, you will already need to hold an RN license. Many programs also specify that you have two or more years not just of nursing experience, but also in nursing experience specific to pediatric primary or acute care.
How much do pediatric nurse practitioners make?
According to the Bureau of Labor Statistics, the median annual salary for nurse practitioners in 2020 was $111,680. Those in the top ten percent of the profession could bring home $156,160 or more.
BLS doesn’t separate the data to specifically cover pediatric nurse practitioners. It’s very likely their salaries are in line with the profession as a whole, or even slightly above the median due to the specialized nature of their training and practice area.
What is the role of pediatric NPs in a pediatric ward?
Working at a peds ward in a hospital environment means you are working with some of the sickest and most vulnerable patients a pediatric nurse will ever have to deal with. Advanced practice nurses have more advanced skills, which also means they take on more responsibility for those patients. PICU and NICU nurses carefully monitor patients both through electronic sensors and by regularly checking them physically. They also take those opportunities to reassure and encourage their patients, who need that contact and care far more than adults. And pediatric ward NPs also perform the full slate of diagnostic testing and treatments needed for their patients.




